Rich Raymond, RN
Rich Raymond, nurse manager of the Burn ICU and Vascular Access at Mercy Hospital in Springfield, Missouri, recently participated in a webinar, PermeaDerm® Biosynthetic Wound Matrix for Partial-Thickness Wound Management. He showcased two clinical cases and explained how and why his team chose to adopt PermeaDerm.
The following is a shortened transcript of the webinar, including his team’s experience with PermeaDerm and how it has transformed their treatment protocols, and three noticeable benefits of using a biosynthetic wound matrix: transparency for wound progress visibility without manipulation, single application that aids in sending patients home sooner, and patient feedback reporting a reduction in pain.
If you prefer to watch the full, recorded webinar video, you can view it here.
Moderator: Today, we’re very pleased to welcome our featured speaker, Rich Raymond. Rich Raymond is the dedicated nurse manager of the Burn ICU and Vascular Access at Mercy Hospital in Springfield, Missouri. With an impressive 27-year career, Rich has excelled in direct patient care, leadership, and operational oversight within this renowned Level 1 Trauma and Burn Center.
Rich Raymond: Hello, everyone. It’s nice to be with you on the call today and webinar. Thanks for the introduction. Again, my career has been entirely spent really in providing care to burn patients in our region. Mercy Hospital is a renowned hospital in southwest Missouri, and our burn center serves quite a large area in this area, including areas of Kansas, Oklahoma, northwest Arkansas, and then a large portion of southern Missouri.
We are very busy at our burn center and have a lot of experience in multiple treatments and care that’s provided for these types of injuries. We admit approximately 300 patients to our burn center, but ever increasingly from year to year, we are trying to move patients to more of an outpatient setting to care for them whenever that’s appropriate and a lot that occurs as we advance products and treatments for burn patients that we’ve not had before.
Today, I’d like to share with you one of those treatments that we’ve used for many, many years. Something that we have been very successful with here at Mercy-Burn Center is the use of a product called PermeaDerm. And again, I would just like to share my experience and the experience of our provider team and nursing team in treating these patients with this product very successfully, and how we’ve been able to gain that advantage in length of stay and patient satisfaction.
PermeaDerm really has a lot of indications. Primarily, we’ll focus on the indications as we use it here in the burn center for acute partial-thickness wound injuries. But some of the indications are for partial-thickness burns, as well as wounds, donor sites, surgical wounds, and can also be used over meshed autographs, as well chronic wounds.
In our experience with PermeaDerm, we have used this on over 200 patients in our burn center, and we continue to use it whenever patients present and are appropriate for this type of treatment. We started using it because we needed something for this very tricky but common injury.
We all know that partial-thickness burns are predictable and they usually heal, but there’s also a predictable amount of time that there’s a lot of pain. And so how can we accomplish something that will heal without surgical intervention? But there are also complications along the way with pain control, dressing changes, and involvement of the care team. So how do we get a dressing that really helps to alleviate some of those things in this partial-thickness type of injury? That’s where PermeaDerm has really worked well for us.
The problem with using traditional dressings outside of PermeaDerm is the dressings themselves. They’re painful. They’re usually changed daily or every other day. There are some products that can allow you to go a little bit lengthier amount of time with some silicone-based products. But there is still a manipulation of the wound bed and some other generalized treatment modalities that still occur with those traditional dressings. For us, that’s where PermeaDerm has worked and has worked out well.
It has a lot of key features that are really key to the treatments that we’re looking for and the goals that we are looking for. Transparency – this allows direct visualization of the wound bed without manipulation. Once applied, that clinician or provider care team can see what’s going on with this wound bed without additional manipulation.

Additionally, we know that burns and wounds occur in complicated areas over joints and contours. This product is flexible. It has a silicone-based backing that allows for some protection once it’s applied. But that inner layer does really help with that intimate contact and early mobilization with that flexibility.
And it also has some customized moisture management. We all know that acute burns have a phase where there’s a lot of drainage and that occurs in that inflammatory process, those first few days, 24 to 48, even up to 72 hours. Managing that moisture can be kind of complicated, especially if you’re putting what seems to be an occlusive type of dressing on the product. This is not an occlusive dressing. It actually allows for some customizable moisture management to allow for that exudate to move through the product. Also, it allows for ambient air exchange.
Eventually, with this product, it will dry and lift away to a completely re-epithelialized surface. And it does that in the appropriate setting, in the appropriate placement, in the proper wound choice. Our providers and our care team here have found that to be consistent and that’s why we continue to use it and have the success that we’ve had on the patients that we have been treating with it so far.
Biosynthetic wound matrix clinical cases
Case 1: Pediatric scald injury
I do have a few examples I’d like to share with you clinically. This is one of our patients. It’s a pediatric patient, a two-year-old female that presented with a 3% partial-thickness scald on the anterior thigh. When this patient came in, they came in through the emergency room. The wound was debrided through light debridement and then PermeaDerm was applied to the thigh.
As you can see in the initial presentation, in the photo, the wound bed is very characteristic of a partial-thickness burn. You see pink tissue there. You see a shiny surface, which indicates some moisture. If you were able to actually touch this wound, you could visualize capillary refill. All those things indicate that we’ve got a burn that is likely partial-thickness and will heal with appropriate care.
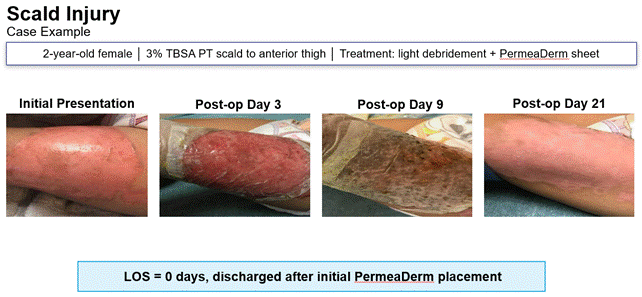
Our team elected to go ahead and use PermeaDerm in this instance because of the presentation and the appropriateness of the product. It was applied in the emergency room to this wound in entirety. The care team used one single sheet of product to try to cover the entire surface. This patient was sent home, and we do occasionally do that on smaller surfaces where we feel like there’s good support and the patients are able to have a video visit if it’s a long way away, or they’re able to come back into our clinic. We do send patients appropriately home for follow-up and clinic. This patient was sent home on a post-op, post-placement day three.
I came back to the clinic and this was the presentation of the product. And this is really good to really talk through and explain because this is typically what we see when we apply PermeaDerm. What we’re looking for is a good adherence. Minimal wrinkles and bubbles and it’s flexible when the patient moves. Now this did not extend over a joint but even as the patient moved there are skin changes that happen even in the thigh. And the product is flexible even when doing that. And this is a two-year-old! So it even remained intact on a two-year old.
On post-op day three if you can see in that one there are a few bubbles; small bubbles on the left-hand side of that photo – those sometimes occur. If there is an area of fluid accumulation or air exchange that didn’t migrate through the fenestration, that may occur. At our clinic day, what we do is assess and evaluate those wrinkles and bubbles. We’ll take the small scissors, sterile scissors, and just open up that spot and lay it back down. Same on the wrinkles as well. Try to lay those back flat again and reapply the dressing.
This patient was sent home on day three from the clinic with dressings reapplied. Post-placement day nine, again, this is textbook, what we typically see with our PermeaDerm placements. It’s very dry, it’s still adherent but very dry. And that indicates that the majority of that wound bed has re-epithelialized underneath and it’s an appropriate time to look at potentially removing the product.
Most of the time… When it occurs, this healing occurs, like you see in post-op day nine, the product will begin to kind of lift at the edges. It’ll be very dry and kind of lift and flake away. And we know at that point it’s time to really help encourage that removal. That’s a manual process. It can be done very gently and judiciously there at the clinic or whatever setting it is. It’s generally not painful. It usually comes off very easily.
If there is any need to facilitate removal because of any dry drainage to hair that may be growing or anything like that, we will apply an emollient to the edges; there are a multiple number of different types of emollients, but just something as simple as Vaseline or Aquaphor can be used at the edges and massaged with a finger to help soften and remove that. It’s important in removing this product that at any point we notice any bleeding, we will stop at that area. We’ll move to another area and leave that in place. That re-epithelialized skin is very thin and fragile, and we don’t want to tear or open that, so we’ll leave that a few days.
But in general, this is the typical healing of a partial-thickness wound. What’s been great during this entire time, even though it’s been nine days, for the family and the patient, there was really not much else to do after the application. That product was left in place. It was secured and covered with some basic simple dressings. The care needed by our provider team, our nursing staff, and I’m absolutely sure from the family, and the parents caring for this wound, and on a two-year-old, they were very thankful they didn’t have to completely remove dressings and wash a wound bed with a child that is not understanding.
And you can see on post-op day 21, this was just a follow-up clinic visit, you see just the appearance of this wound after PermeaDerm has been removed. Healing, not open. We don’t see really any scar formation. This is soon for scars, but the color, the pliability, redness, all those inflammatory markers really are not there. At post-op day 21, this patient looks great.
Case 2: Partial-thickness to deep partial-thickness scald injury
I do want to move to another patient that we’ve treated. The patient was an 82% partial-thickness and mixed depth deep partial-thickness scald injury that presented to us.
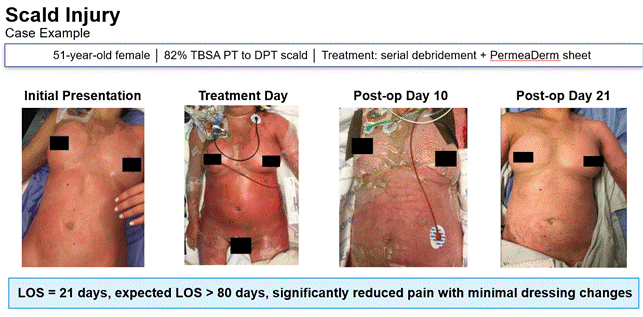
She was intubated and somewhat complicated initially on her admission, given her size of burn and the things that were going on with that physiology that occurs with any large burn. But this patient, we debrided, evaluated; our provider team and nursing staff worked closely together to really evaluate again what product would be best to not just look at the now, but also in the future. What’s the treatment tomorrow, two days, three days, four days going to be like for this patient with this large burn? How do we minimize additional patient movement, metabolism issues, hypothermia, with taking dressings off, a whole host of things with not just the now, but in the future.
We elected to place PermeaDerm on her burns, knowing that some of them were slightly deeper and may eventually need grafting. You can see the initial presentation, treatment day that we applied it. What is not included in these photos, but also was successful in this treatment, was her legs were also circumferential for the most part; her left leg particularly was a circumferential partial-thickness burn. And PermeaDerm was placed on that in entirety as well. The only place that PermeaDerm was not placed was her back, and that was treated with a different silicone product. The reason we did not use PermeaDerm on her back was because of her condition. Otherwise we would have. Rolling her and moving her caused some cardiac and pulmonary complications, and we just needed to keep her as flat as possible during the application of the product.
So this product was applied to the majority of this patient’s surface. On post-op day 10, you can see some residual PermeaDerm, and we’ve had some areas on her abdomen that have been healed. We have some on her breast that are still intact, but you can that that’s drying on post-opt day 10 wherein it’s still adherent. It’s like we would like to see. There are some wrinkles in that product, but that’s over areas that really were not damaged by that thermal injury. We didn’t really manipulate that much, but you can see it’s healing well post-op day 10.
We also know that everyone heals at a different rate. There’s some general guidelines, but depending on the depth, the overall health, the location, a multitude of things, the date of removal will vary; age of the patient, there’s a lot of variables in the date that this will come off. But there is some predictability, and if it is a partial-thickness burn, we do have some guidelines. And our providers just evaluate that when these dressings are taken down.
The outer dressings were taken down to kind of see where we’re at in healing. And again, the beauty of our use with this product is the non-manipulation of the wound bed. Our providers and care team can see what’s going on underneath this product without any type of manipulation. And for our patients, it’s wonderful as well. Here we have on post-op day 21, and again, the legs are not included, all of the PermeaDerm has been removed and all of her surfaces have re-epithelialized with PermeaDerm.
There were a few places that did convert to a full-thickness area that required grafting. We anticipated that though, at the beginning – we could see those changes and elected to use PermeaDerm. The providers just windowed out those areas as they declared themselves as when Parmeoderm did not stick. It’s very indicative of areas that are likely potentially are full-thickness or a deep partial that should be treated locally.
Overall, this patient did have to have about 8% of her burn that required grafting, but it was an amazing result, we feel, for the use of the product in a very large wound burn injury that is not commonly presented in a lot of cases. So very good success. And for us as a care team to minimize those daily or sometimes multiple dressing changes per day, I know really gave us some advantages in getting her extubated and actually discharged close to day 21 to the outpatient setting. And that’s quite amazing, even for a partial-thickness burn that’s 82 percent. To be discharged around day 21 from admission to acute care center is quite amazing and we really do attribute it to our product choice in this instance knowing that we did have some areas that needed some differing treatment.
Why and how they adopted PermeaDerm
So let me just help whoever’s on the call if those are asking, and I briefly alluded to, why did we want to do this? We needed a product to kind of accomplish multiple things. It’s been a multifaceted product to accomplish many things, and we’ve seen that.
But where did we start using it? It was really, honestly, scald injuries. That’s where we began using Permeaderm and had the best success because it was pretty much straightforward. Unless the scald had, and we still use it in these instances, but not initially, scalds that are just water. Scalds that are heavy with oil in them like some pastas or soups can actually hold on to heat significantly and will result sometimes in a deeper burn, but we started with scald. That’s where we learned how to use this product. We had tremendous success.
Our physicians, our nursing team saw it immediately. Our patients felt it immediately in the pain control. Pain control, we shrugged a shoulder at it because we’re like, eh, how can it do that? We absolutely saw a significant difference in reports of pain once this was applied to a partial-thickness injury. And as clinicians, we all know that these injuries are honestly some of the most painful. These partial-thickness injuries that we’re, like, oh, that’s not bad. It’s not, in that it should heal without significant surgical care or treatment. But for the patient, they hurt, they’re painful. It’s very, very distracting, very, very uncomfortable. And sometimes we lose sight of that. How can we moderate and alleviate that?
Back to why we used it. Scald is where we started. And from there, we really, once we got that comfort level, we began to move into those areas that were slightly deeper partial-thickness injuries, you know, knowing that there are zones of deeper depth. Let’s go ahead and use the PermeaDerm on it. You know, we’ll watch that area. Sometimes it will go ahead, and for lack of a better word, temporize that area and the product will work. There have been times that that area has not stuck and we’ve just windowed it out, but we’ve anticipated that. And the majority of the wound has still been treated with PermeaDerm. And all we’re treating is a small focal area as opposed to the large surface.
And we’ve also moved to donor sites. Donor sites is another great place to really talk about because that as well is a known depth. Our surgeons and physician assistants, nurse practitioners helping that surgical suite, they dial in the depth. You know exactly how deep that skin injury is going be and it’s partial-thickness unless there’s a mistake that is a partial-thickness injury. And PermeaDerm is a great application in those donor sites; small donor sites or donor sites that you can apply the product to really help with that wound healing just as we treat those partial-thickness burns.
The other area that I’d say our center has gravitated into after that initial comfort level and success were more abrasions, wound type injuries, abrasions or other skin conditions that cause some loss or denuding of skin. The thing about abrasions though is back to the key, these have to be clean. So if there’s an abrasion that’s filled with a lot of gravel or dirt that cannot be cleaned, it’s not an appropriate application. The wound bed absolutely has to be clean without biofilm products or debris in it to be effective. Otherwise, potentially you’re setting that patient up for an infection, not because of the product, but because of that closed nature of that wound environment that you’re creating without ensuring that wound bed is nice and clean.
Looking for more content like this? Read PermeaDerm as a Sound Option for a Primary Wound Matrix or Modern Burn Care: Targeted Solutions to Optimize Patient Recovery.

About the author
Rich Raymond, BSN, RN, is the dedicated Nurse Manager of the Burn ICU and Vascular Access at Mercy Hospital Springfield, MO. With an impressive 27-year career, Rich has excelled in direct patient care, leadership, and operational oversight within this renowned Level 1 Trauma and Burn Center.
Mercy’s Burn Center serves as a beacon of hope for burn patients across Southern Missouri, Kansas, Arkansas, and Oklahoma. Rich and his passionate team are committed to providing exceptional burn care and continually strive to advance the field. They leverage their expertise to evaluate and implement innovative technologies and treatments, accelerating recovery and improving patient outcomes.
The views and experiences described above are the author’s own and may or may not reflect those of AVITA Medical.