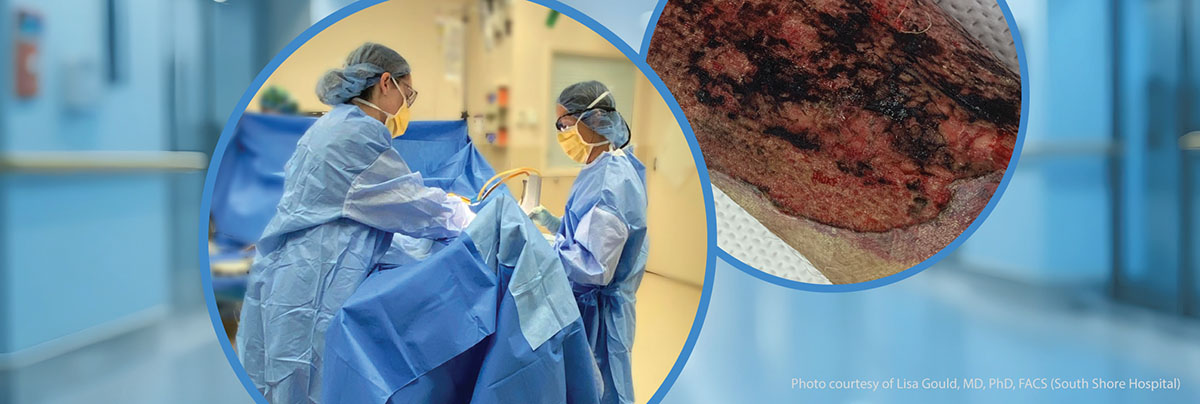
Lisa Gould, MD, PhD, FACS
Early in my training, plastic surgeons were considered the “surgeons’ surgeon,” meaning that when all else failed, the plastic surgeon might have an answer to ‘fill the black hole.’ That is still true in my role as the Wound Surgeon for our community hospital.
But things have changed in terms of the acuity of patients.
Patients in the hospital or those who seek care in wound centers are older and sicker than they were 25 years ago. There is increasing pressure to reduce hospital length of stay, and insurance companies have more say about what they will pay for, including transitions of care. This means that we need to be very thoughtful about surgical planning, coordination of care and utilizing available resources.
Wound care challenges
I am often called upon to evaluate patients over the age of 80 with large leg wounds after hematomas or other traumatic injuries. Skin grafts are the standard of care for definitive closure of deep partial or full-thickness wounds, however, they require a donor site that can be painful and slow to heal. Furthermore, many of my patients are anticoagulated and have fragile skin, making both the donor site and the wound difficult to manage.
Evidence-based wound care improvements
As a long-term member and past president of the Wound Healing Society, my focus has always been on evidence-based wound care. As a wound surgeon, my goal is to get people healed as fast and expeditiously as possible.
My experience and training have led me to be skeptical about new products, as there is rarely anything truly new and exciting that has made it through clinical trials for wounds. Yet there has been one innovation that has truly changed my practice.
Skin cell suspension autograft
The innovation I am referring to is RECELL® technology that converts a thin piece of skin into a single cell suspension, i.e., autologous skin cell suspension (ASCS). This point-of-care technology has the advantage of reducing donor site morbidity, both in terms of size, scarring, and time to closure, which is really valuable for my older adults.
Although it was initially approved for thermal injuries in 2018, it was later approved for non-thermal injuries in June of 2023, and I treated my first patient in August of 2023. Since then, I have treated more than 30 patients with ASCS. Most of these are lower extremity wounds, four were bilateral and about half are in patients over the age of 70, many of whom are anticoagulated.
I have not abandoned traditional split-thickness skin grafts, but have identified the patients who will benefit most from ASCS, including those with multiple comorbid illnesses, large wounds for whom the donor site would be extensive, patients with pain that is difficult to control, especially in patients with substance use disorder, and people with fragile skin related to age or other clinical conditions. The majority of my patients are treated in the operating room on an outpatient basis, and the results are compelling both in terms of healing and cosmesis.
My experience is that the donor site is much less problematic – most are healed within 10 days, and I no longer get calls about the patient going to the ED because of bleeding from the donor site. I see my patients weekly, and on average they require four post-op visits. I only needed to re-graft three patients and they healed after that.
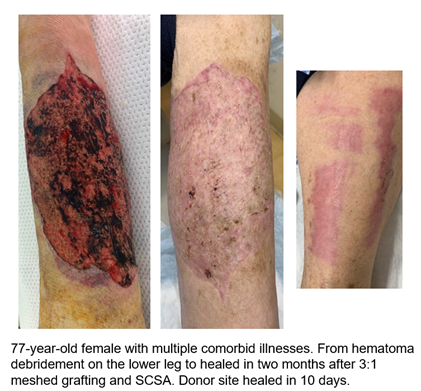
Reducing wound care requirements for earlier discharge
Patients with wounds are medically complex and require extra care, both pre- and post-operatively, to ensure that they heal without further complications. Previously, these patients would require potential hospital re-admissions and multiple doctor visits. With this technology in my toolbox, patients can be discharged from the hospital earlier with reduced wound care requirements. Additionally, the wounds are closed expeditiously, decreasing resource utilization at multiple levels.
It is a challenge to cross the chasm for adoption of new technologies. As an early adopter I can truthfully say this technology has changed my practice. One of my goals is to disseminate this information so that others can benefit as I and my patients have. However, at the same time, we need to continue to innovate, explore new indications, and consider ways to improve upon the current technology. Surgeons tend to be skeptics, requiring data rather than anecdotes. This product meets that criteria, but more research based on end-user input will lead to improvements that can heal more patients.
Looking for more like this? Read Beyond Wound Closure: Restoring Form, Function, and Quality After Traumatic Injury or Re-Seeding Wounds: Fast-Track Healing and Skin Renewal.
Or learn more about RECELL® autologous skin cell suspension.

About the author
Dr. Lisa Gould earned her MD, PhD in the Medical Scholars Program at the University of Illinois at Urbana-Champaign. She has been practicing plastic and reconstructive surgery with an emphasis on difficult wound problems since 1999. She is an Affiliate Professor in the Department of Molecular Pharmacology and Physiology at University of South Florida, Clinical Associate Professor of Medicine at Brown University and Clinical Associate Professor of Surgery at Tufts University School of Medicine. Dr. Gould brings her passion for research and education in wound care to her clinical practice at South Shore Hospital and the South Shore Health Center for Wound Healing in Weymouth, Massachusetts and to the national organizations that she serves, including the Wound Healing Society, the Alliance of Wound Care Stakeholders, the National Pressure Injury Advisory Panel, the MAVEN project, the Wound Care Collaborative Community and the American College of Surgeons.
The views and experiences described above are the author’s own and may or may not reflect those of AVITA Medical.